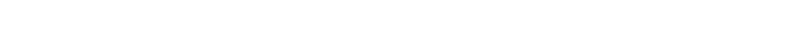Within days, Virginia’s hospitals likely will be caring for the highest number yet of COVID-19 patients and further risking the physical and mental health of fatigued caregivers.
On Nov. 1, the seven-day moving average in Virginia for hospital patients with the virus was just above 1,000. By mid-month it has climbed to 1,250, and within 10 days it stood at 1,516. That was Wednesday, Thanksgiving Eve, the day when all across the state and country people ignored public health warnings and traveled to spend the holiday with families.
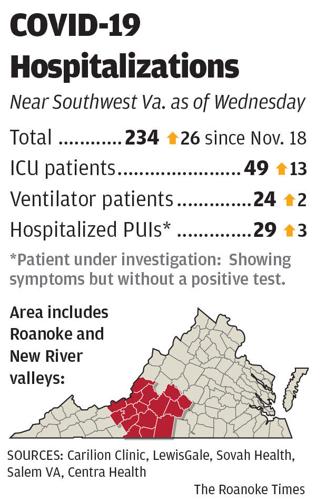
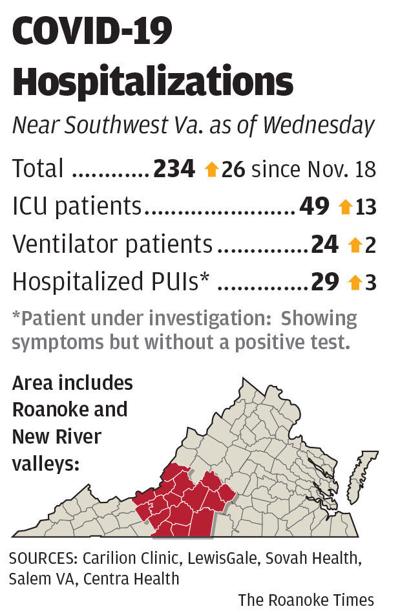
It was a day hospital systems across the Roanoke and New River valleys reported a 15% increase in COVID-19 patients from the week before, from 208 to 234, and a 36% jump, from 36 to 49, in the number of patients who required intensive care.
“The numbers are going in the wrong direction. We can’t say it any more clearly than that,” said Julian Walker, spokesman for the Virginia Hospital and Healthcare Association. “We have the dashboard that every day says these are the numbers. No one is hiding he ball here. Everyone is being very clear in saying this is a problem.”
People are also reading…
Virginia’s hospitals hit their peak of virus patients on May 8 with 1,650. On Wednesday, 1,549 hospital beds statewide were filled with COVID-19 patients, with health officials worried about a post-Thanksgiving surge.
“The reality is people are going to do what people are going to do. That may not be the wisest decision that people are making. That’s free will,” Walker said. “All we can do is vigorously and vehemently encourage them to be safe and to be smart.”
Dr. Cynthia Morrow, director of the Roanoke City and Alleghany Health Districts, made one last pitch earlier this week for people to hunker at home instead of traveling and to eat their meal only with people who live with them.
“We expect our numbers to go up exponentially. I hope that I’m wrong. I really hope that I am wrong,” she said. “If people do the right thing, we may not see this trajectory that we are all expecting. But for reasons I will never understand, a lot of people don’t seem to want to follow the guidelines which we know are effective.”
Morrow added, “If we all do the right thing, we can prevent what we believe is inevitable.”
Jamie Swift, Ballad Health’s infection officer, was less hopeful. By Tuesday she figured the turkeys had been bought, the plans made.
She worried about a post-Thanksgiving surge.
“We very quickly could get to that catastrophic number we are talking about, stressing the health care system,” she said.
Ballad has already needed to curtail some surgeries and procedures that require overnight hospital stays in order to turn more and more of its units over to caring for COVID-19 patients. The region it serves in the far southwest corner of Virginia and the northeast corner of Tennessee had reported its highest number of deaths since the pandemic began came in November. As of Wednesday, 94 people had died in the last seven days.
Also Wednesday, 210 patients with the virus were in Ballad hospitals; 43 of them required intensive care and 26 were on ventilators. The count was down slightly from the week before, but Ballad looks at the number of new positive tests in the community — which hit the highest yet last week — and knows that within five to 10 days, between 7% and 9% of those people will become so ill they will be admitted.
The cases have been surging in Ballad’s region for more than six months. Its executives, team members, patients and families have pleaded during weekly Facebook Live videos for people to wear masks, keep their distance, stay home if they are ill.
Not all heed the warning.
Swift said she knows everyone is tired. She’s tired, she said, but she’s going to keep saying the same things, hoping people hear.
“I don’t know what it’s going to take to convince people. What I hope it doesn’t take is for them or their family member laying in the ICU,” she said.
On Nov. 18, Alison Johnson, director of critical care at Johnson City Medical Center, said, “We are depressed, disheartened and tired to the bone.”
She said she wished those shunning masks and disbelieving science could see and feel the fear of patients and the anguish of their families who cannot visit.
“We see your posts, and we hear you talk and it undermines and belittles our calling,” she said. She and her colleagues try to brush it off, she said, but there are days they cry on the way to work, and days they cry on the way home.
This week Ballad reported that 220 of its staff members were in isolation or quarantine after being exposed to the virus.
COO Eric Deaton said Ballad was able to hire about 60 or so new team members but remains very concerned about staffing. The system struggled with a nursing shortage before the pandemic, and has been offering bonuses and raises.
He said they are very concerned about staff burnout.
“To put everything bluntly, we could run out of resources,” he has said. “Our most precious resource is our team members.”
“Health care workers are exhausted,” said Sherry Kolb, president of Qualivis, which works with state hospital associations and health systems to connect them with travel nurses and allied staff agencies. “When you think about a typical crisis, you think about hurricanes. You think about natural disaster, where you need to get folks in quickly and help either support the staff or relieve the staff. But what we are seeing now, nurses either want to follow the pay and those kind of logistics, or they want a break. Something we never experienced before.”
Kolb said the demand is so strong now for travel nurses that hospitals across the nation needed more than 27,000 last week, and Virginia hospitals had 866 open jobs.
“The demand is not concentrated to a few pockets like we saw in the first wave of the coronavirus. We are seeing the demand nationally,” she said. “I think a lot of people are worried that we don’t have enough nurses. The truth of the matter is there are more nurses. But the nurses are able to truly choose based on where they want to go.”
She said her firm is advising health systems on how to streamline their hiring process and how to make their assignments more attractive.
Walker, with Virginia’s hospital association, said having enough personal protective equipment and testing isn’t as large of a concern as it was at the start of the pandemic, and with months of experience, each system is better at managing other services while caring for increasing numbers of COVID-19 patients.
But staffing remains a challenge, he said.
Dr. Daniel Carey, the state’s health secretary, said earlier this month that with other types of disasters, hospitals could lend each other staff. But that’s not an option now. If Ballad has more patients than it can care for, Carey said some might need to be transferred north on Interstate 81 to other health systems.
Walker said that is last-resort planning.
“Look, we’re talking about all options. In an unusual situation like this, we have to consider all options,” he said, noting it was similar to the plan to open field hospitals at the start of the pandemic.
“While that planning process was fully realized, the facilities weren’t opened because it wasn’t necessary,” he said.
The governor last week imposed more restrictions on the number of people who can gather publicly, and ordered restaurants and bars to close early.
Behavior modifications can work to control the virus, public health officials said, but changes take about two weeks to affect the number of infections, and then another week or two to show up in hospitals admissions and deaths.
The rise in cases was predicted in early October as public health officials warned of colder weather prompting people to go indoors to socialize in poorly ventilated spaces, and of the coming holidays.